E. Coli Gut Bacteria
It’s likely that you have heard someone express the feeling of having “butterflies” or a “knot” in their stomach. You have probably also heard someone tell you to “trust your gut” in response to your intuition or instincts about a strange situation. However, what you might not know is that these bodily experiences are not inexplicable or random, but are in fact a result of a real connection between your gut and your brain which has an impact on your overall health. Not only is this connection more tangible than many realize, but you also have some level of control over it and how it affects your gut-brain health.
Your gut and your brain are deeply intertwined by a connection called the gut-brain axis. The gut brain axis has two main parts: the central nervous system and the enteric nervous system. Your central nervous system is made up of your brain and spinal cord, whereas your enteric nervous system refers to the hundreds of millions of neurons, or brain cells, which line the inside of your gut, or gastrointestinal, walls (1, 2). There are more neurons in your gut than there are in your whole spinal cord (3)! These neurons in your gut are important for sensory reasons, allowing your brain to send sensation to your gastrointestinal tract and moderate its function.
The fitness of our gut can be measured by taking a closer look at the organisms that live inside our gut, this is called the microbiome (4). Your gut microbiome is comprised of both beneficial and harmful bacteria, primarily in the intestines. There are thousands of types of bacteria in your gut, and it is estimated that there could be up to 100 trillion total bacteria within your gastrointestinal tract (5). Everybody has a unique gut microbiome, which operates like its own ecosystem, but people with healthy gut microbiomes have comparable amounts of good bacteria to one another (1). Having too much or too little of a particular gut bacteria can throw off your gut ecosystem. Your gut bacteria send out chemical signals that have an impact on your health, both physically and mentally. For example, some of the chemical signals most commonly produced by gut bacteria contribute to proper brain and gut function, promoting a stable mood, regulated gut movement and digestion, a strong immune system, stomach acid levels, and a reinforced gastrointestinal barrier (6, 7, 8, 9, 10). As important and beneficial as these chemical signals are, having too much or too little of any of them can lead to physical symptoms like immune system dysfunction, gut inflammation, over-production of stomach acid, and psychological symptoms like increased stress, anxiety, and lowered mood (9, 10).
About 20% of people in the United States over the age of 18 experience anxiety or depression (11). Despite how common these neuropsychological disorders are, many do not realize the role your gut health can play in their symptomology. Many people believe that psychiatric disorders, as the name suggests, are centered exclusively around dysfunctional psychological processes, occurring only within the mind and brain. However, your gut microbiome plays a significant role in regulating your mood and therefore your levels of depression and anxiety. There are multiple gut bacteria that have been linked to depression and anxiety symptomology, as well as overall higher stress and decreased mood. One type of gut bacteria that has been associated with decreasing the symptomology of these psychological disorders is Lactobacillus, which we can call Lacto for short (12). Lacto is a good bacterium, which are often referred to as probiotics, that helps your gut by aiding in digestion, nutrient absorption, and promoting the growth of more healthy gut bacteria (13, 14). People with disorders like depression and anxiety have been found to possess smaller amounts of Lacto in their gut microbiome, with psychologically healthy individuals possessing greater amounts (15, 12, 16). On the other hand, Klebsiella, or in our case, Kleb, does the opposite. While psychologically healthy individuals have lower amounts of Kleb, increased Kleb numbers are commonly found in individuals with anxiety or depression, with Kleb contributing to mood imbalances, digestive issues, and inflammation (16, 17).
Disorders of the gut-brain axis are extremely common. It is estimated that about 40% of people in the United States over the age of 18 have a disorder of the gut-brain axis, and the most common of these is irritable bowel syndrome, or IBS (18, 19). There are multiple types of IBS, but the primary symptomology of IBS as a whole includes abdominal pain and constipation or diarrhea that has an adverse effect on life quality and function, and has also been associated with depression and anxiety in almost 70% of patients (20). The pain associated with IBS had been researched using fMRI technology, a brain imaging method which allows scientists to see the brain areas activated by IBS-related pain using a glowing tag injected into the bloodstream (21). IBS can also affect sleep quality and cause fatigue (18). People with IBS have not only been found to have lower amounts of Lacto, just as those with anxiety depression do, but higher amounts of E. coli bacteria are also present (20). When present in large numbers in the gut, E. coli contributes to the symptomology of IBS by preventing cells in the gastrointestinal tract from adequately absorbing water and damaging blood vessels within your intestines. E Coli can also release toxins into your gut that hurt gastrointestinal cells (22).
| Bacteria Type | Function |
| Lactobacillus | Absorbs nutrients, aids digestion, promotes good bacteria growth |
| Klebsiella | Mood imbalances, gut inflammation, digestion issues |
| E. Coli | Prevents water absorption, releases toxins, damages blood cells in the intestines |
Your sex can also have an effect on your gut health, with females being disproportionately affected by disorders of the gut-brain axis and experiencing more debilitating symptoms on average (19, 20, 23). Women experience IBS at almost double the rate of men, and sex differences in gut microbiome and hormones are the root of this difference (23). Females with IBS have been found to have larger amounts of bacterial diversity than males with IBS, including greater numbers of toxic, harmful bacteria. This difference in gut-brain axis regulation may be due to environmental and genetic factors, as well as how female sex hormones fluctuate across the menstrual cycle (24). During menstruation, when the sex hormones estrogen and progesterone are at their lowest, women experience more severe IBS symptoms, including bowel issues and serious abdominal pain. Additionally, during the phase where estrogen and progesterone levels quickly decrease from their peak, the same increase in IBS symptoms is experience, alongside more severe bloating (25). These symptoms can be debilitating to sufferers of IBS and other disorders of the gut-brain axis. But how do the bacteria in your gut tell your brain about the status and health of your gut?
The gut and brain are connected via the vagus nerve. The vagus nerve is the longest nerve in your body that starts at your brain, stretching from your throat, through your chest, to your lungs and heart, and into your digestive tract in your abdomen (26). The vagus nerve serves as a pathway for two-way communication between your gut and your brain, acting as a telephone line that connects them. By sending information through the line, gut is able to tell your brain about the chemical signals being released by your gut bacteria, and your brain can respond appropriately. Your brain can also tell your gut how to function, letting it know when to digest and to respond to danger with discomfort. Because your vagus nerve plays such a key role in brain to body communication, reaching many vital organs within the body, it is an extremely important part of your parasympathetic nervous system.
When someone has a “fight or flight” response, their heart rate will increase, they will breathe more quickly, and their digestive processes will cease as the body prioritizes its energy for defending against danger (27). On the other hand, there is the parasympathetic nervous system, which aids in “rest and digest” body processes and is activated when you feel calm and content. When your parasympathetic nervous system is active, your brain will use the telephone line to tell your heartrate to slow, your stomach to digest, and your body to conserve energy rather than expend it (27). Your vagus nerve is a key player in these “rest and digest” functions, delivering messages from your brain to your organs about when it’s time to slow down and relax. Because it is involved in the stress response, the vagus nerve is sensitive to stress. When you are feeling anxious, upset, or have an otherwise low mood, your brain uses the telephone line to communicate this to your internal organs. In the case of your gut-brain axis, this means your stomach might experience discomfort, with your digestive processes ceasing and that metaphorical “knot” forming. Your microbiome can also tell your brain when your gut is unhealthy, which causes your brain to become stressed and results in the same discomforting outcome (28). When your vagus nerve is damaged or dysfunctional, it can result in a plethora of adverse health conditions, including neuropsychological disorders and disorders of the gut-brain axis.
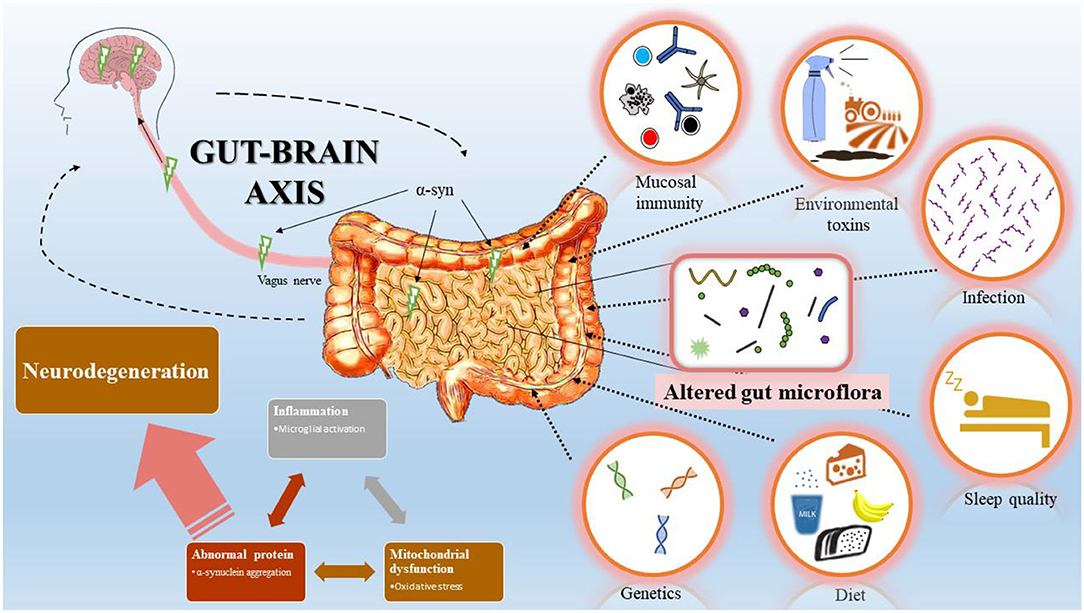
While there are many negative effects of poor gut-brain health, the good thing is that we do hold some control over it. There are changes we can make to our lifestyle to improve the health of our gut-brain axis and the gut microbiome that helps govern it. Previous research has suggested that there are a few primary components to maintaining positive gut-brain health that we all have the power to incorporate into our lives. These include leading an active lifestyle, eating right, getting good sleep, and adequately managing stress.
Exercising and staying active plays an important role in maintaining your overall gut-brain health. While exercise has been shown to have direct effects on brain health, including protecting brain areas associated with important cognitive functions like attention and memory, it is also beneficial to the bacteria that form your gut microbiome. Doing aerobic exercise or cardio has been shown by scientific literature to help diversify the bacteria within the gut and promote healthy gut function, as exercise aids digestive processes and promotes blood flow to the gut (29). These improvements in gut function have been linked to positive changes in both gut and brain health. IBS symptoms such as bloating, abdominal pain, and indigestion are decreased when you exercise. Exercise also lessens feelings of anxiety, depression, and stress (30)
Your diet is also a major contributor to your overall gut-brain fitness. Maintaining a healthy, balanced diet improves your gut-brain health and can promote the growth of good gut bacteria while decreasing the presence of bad ones. For example, probiotics like Lacto can be used to prevent the growth of a bad gut microbiome, aiding in digestion and decreasing stomach discomfort, and can be found in foods like yogurt, sauerkraut, cheese, and sourdough (31, 32). Prioritizing your intake of whole foods, foods that are high in fiber, and foods that are low in fat are a great way to maintain a healthy gut as they provide your good gut bacteria with adequate nutrients. Good foods for your gut microbiome include sweet potatoes, mushrooms, beans, and fruit. Contrastingly, foods that are high in fat, heavily processed, and nutrient deficient, like pizza, donuts, and deli meats, should be avoided, as they promote the growth of harmful gut bacteria (33, 34).
Quality sleep is important for your body to function properly, and your gut health is no exception. Being deprived of sleep is detrimental to your gut microbiome, changing its composition in harmful ways that lower its diversity, whereas good sleep promotes good microbiome diversity through the same means as exercise (35). Quality sleep has also been shown to support your gut’s immune system, decrease the presence of proteins in the gut tied to stress-induced inflammation, and foster a gut microbiome that protects your cognitive health and ability to perform tasks of recall and risk assessment (36). Finally, achieving quality sleep is important to maintaining a stable, positive mood (37). 7-9 hours of quality sleep every night, which includes little exposure to light and screens, is recommended for a healthy gut microbiome (38, 36).
Finally, managing your stress levels is crucial to maintaining a healthy gut microbiome. Stress can be detrimental to your gut microbiome, decreasing the presence of good bacteria and inducing inflammation within the gut. This has negative effects on your immune system that make you more susceptible to disease. Additionally, stress contributes to decreases in mood associated with depression and anxiety, which can further disrupt the gut-brain axis (39). For this reason, it is extremely important to lessen the amount of stress in your life, or at the very least, how it affects you. Stress management techniques such as breathing exercises, yoga, meditation, and relaxing through a hobby are great ways to reduce your stress levels and achieve a healthy gut (40).
The gut and the brain have a very real connection to each other, acting on one another and regulating the body’s function. Your gut microbiome is incredibly important to your overall health, including the health of your gut-brain axis and the telephone line, the vagus nerve, which connects them. Without a healthy gut microbiome, both physical and psychological symptoms such as low mood and indigestion can appear, so it is crucial that we take care of our gut microbiomes in every way we can. Even those with brain-gut disorders can benefit from non-pharmaceutical health practices. By maintaining a proper diet, exercising, sleeping well, and managing our stress, we can all keep our gut-brain connection in good health.
References
1. Carabotti, M., Scirocco, A., Maselli, M. A., & Severi, C. (2015). The gut-brain axis: interactions
between enteric microbiota, central and enteric nervous systems. Annals of
gastroenterology, 28(2), 203–209.
2. Furness, J. B., Callaghan, B. P., Rivera, L. R., & Cho, H.-J. (2014). The enteric nervous system and gastrointestinal innervation: Integrated local and Central Control. Advances in Experimental Medicine and Biology, 39–71. https://doi.org/10.1007/978-1-4939-0897-4_3
3. Purves D, Augustine GJ, Fitzpatrick D, et al., editors. Neuroscience. 2nd edition. Sunderland
(MA): Sinauer Associates; 2001. The Enteric Nervous System. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK11097
4. Zhang, Y.-J., Li, S., Gan, R.-Y., Zhou, T., Xu, D.-P., & Li, H.-B. (2015). Impacts of gut bacteria on human health and diseases. International Journal of Molecular Sciences, 16(4), 7493–7519. https://doi.org/10.3390/ijms16047493
5. Ferranti, E. P., Dunbar, S. B., Dunlop, A. L., & Corwin, E. J. (2014). 20 things you didn’t know about the human gut microbiome. Journal of Cardiovascular Nursing, 29(6), 479–481. https://doi.org/10.1097/jcn.0000000000000166
6. Dicks, L. M. (2022). Gut bacteria and neurotransmitters. Microorganisms, 10(9), 1838. https://doi.org/10.3390/microorganisms10091838
7. Guzel, T., & Mirowska-Guzel, D. (2022). The role of serotonin neurotransmission in gastrointestinal tract and pharmacotherapy. Molecules, 27(5), 1680. https://doi.org/10.3390/molecules27051680
8. Hamamah, S., Aghazarian, A., Nazaryan, A., Hajnal, A., & Covasa, M. (2022). Role of microbiota-gut-brain axis in regulating dopaminergic signaling. Biomedicines, 10(2), 436. https://doi.org/10.3390/biomedicines10020436
9. Mazzoli, R., & Pessione, E. (2016). The neuro-endocrinological role of microbial glutamate and GABA signaling. Frontiers in Microbiology, 7. https://doi.org/10.3389/fmicb.2016.01934
10. Smolinska, S., Winiarska, E., Globinska, A., & Jutel, M. (2022). Histamine: A mediator of intestinal disorders—a review. Metabolites, 12(10), 895. https://doi.org/10.3390/metabo12100895
11. Terlizzi, E., & Zablotsky, B. (2024). Symptoms of Anxiety and Depression among Adults: United States, 2019 and 2022. https://doi.org/10.15620/cdc/164018
12. Merkouris, E., Mavroudi, T., Miliotas, D., Tsiptsios, D., Serdari, A., Christidi, F., Doskas, T. K., Mueller, C., & Tsamakis, K. (2024). Probiotics’ effects in the treatment of anxiety and depression: A comprehensive review of 2014–2023 clinical trials. Microorganisms, 12(2), 411. https://doi.org/10.3390/microorganisms12020411
13. Gao, H., Li, X., Chen, X., Hai, D., Wei, C., Zhang, L., & Li, P. (2022). The functional roles of lactobacillus acidophilus in different physiological and pathological processes. Journal of Microbiology and Biotechnology, 32(10), 1226–1233. https://doi.org/10.4014/jmb.2205.05041
14. Cleveland Clinic. (2026, April 17). Acidophilus (lactobacillus acidophilus): Uses, benefits & side effects. https://my.clevelandclinic.org/health/drugs/22650-acidophilus
15. Kumar, A., Pramanik, J., Goyal, N., Chauhan, D., Sivamaruthi, B. S., Prajapati, B. G., & Chaiyasut, C. (2023). Gut Microbiota in anxiety and depression: Unveiling the relationships and Management Options. Pharmaceuticals, 16(4), 565. https://doi.org/10.3390/ph16040565
16. Xiong, R.-G., Li, J., Cheng, J., Zhou, D.-D., Wu, S.-X., Huang, S.-Y., Saimaiti, A., Yang, Z.-J., Gan, R.-Y., & Li, H.-B. (2023). The role of gut microbiota in anxiety, depression, and other mental disorders as well as the protective effects of dietary components. Nutrients, 15(14), 3258. https://doi.org/10.3390/nu15143258
17. Zhang, Q., Su, X., Zhang, C., Chen, W., Wang, Y., Yang, X., Liu, D., Zhang, Y., & Yang, R. (2023). Klebsiella pneumoniae induces inflammatory bowel disease through caspase-11–mediated IL18 in the gut epithelial cells. Cellular and Molecular Gastroenterology and Hepatology, 15(3), 613–632. https://doi.org/10.1016/j.jcmgh.2022.11.005
18. Raskov, H., Burcharth, J., Pommergaard, H.-C., & Rosenberg, J. (2016). Irritable bowel syndrome, the microbiota and the gut-brain axis. Gut Microbes, 7(5), 365–383. https://doi.org/10.1080/19490976.2016.1218585
19. Palsson, O. S., Sperber, A. D., Bangdiwala, S., & Whitehead, W. E. (2023). Prevalence and associated factors of disorders of gut‐brain interaction in the United States: Comparison of two nationwide internet surveys. Neurogastroenterology & Motility, 35(6). https://doi.org/10.1111/nmo.14564
20. Shaikh, S. D., Sun, N., Canakis, A., Park, W. Y., & Weber, H. C. (2023). Irritable bowel syndrome and the gut microbiome: A comprehensive review. Journal of Clinical Medicine, 12(7), 2558. https://doi.org/10.3390/jcm12072558
21. Yuan, Y.-Z. (2003). Functional brain imaging in irritable bowel syndrome with rectal balloon-distention by using fmri. World Journal of Gastroenterology, 9(6), 1356. https://doi.org/10.3748/wjg.v9.i6.1356
22. Ingerson-Mahar, M., & Reid, A. (2011). FAQ: E. Coli: Good, Bad, & Deadly. https://doi.org/10.1128/aamcol.1-2011
23. Kim, Y. S., & Kim, N. (2018). Sex-gender differences in irritable bowel syndrome. Journal of Neurogastroenterology and Motility, 24(4), 544–558. https://doi.org/10.5056/jnm18082
24. Pecyna, P., Gabryel, M., Mankowska-Wierzbicka, D., Nowak-Malczewska, D. M., Jaskiewicz, K., Jaworska, M. M., Tomczak, H., Rydzanicz, M., Ploski, R., Grzymislawski, M., Dobrowolska, A., & Gajecka, M. (2023). Gender influences gut microbiota among patients with irritable bowel syndrome. International Journal of Molecular Sciences, 24(13), 10424. https://doi.org/10.3390/ijms241310424
25. Mulak, A. (2014). Sex hormones in the modulation of irritable bowel syndrome. World Journal of Gastroenterology, 20(10), 2433. https://doi.org/10.3748/wjg.v20.i10.2433
26. Cleveland Clinic. (2026, April 13). Vagus nerve: What it is, function, Location & Conditions. https://my.clevelandclinic.org/health/body/22279-vagus-nerve
27. Giambrone, H. (2025, September 4). Balancing the Nervous System: Insights into Sympathetic and Parasympathetic Roles. Mental Health Center Of San Diego – San Diego’s Premier Mental Health Facility. https://mhcsandiego.com/blog/sympathetic-vs-parasympathetic-balancing-nervous-system-insights/#:~:text=Consider%20stimulating%20the%20gas%20pedal%20and%20the,regain%20normalcy%20once%20the%20stressor%20is%20gone.
28. Ma, L., Wang, H.-B., & Hashimoto, K. (2025). The vagus nerve: An old but new player in brain–body communication. Brain, Behavior, and Immunity, 124, 28–39. https://doi.org/10.1016/j.bbi.2024.11.023
29. Min, L., Ablitip, A., Wang, R., Luciana, T., Wei, M., & Ma, X. (2024). Effects of exercise on gut microbiota of adults: A systematic review and meta-analysis. Nutrients, 16(7), 1070. https://doi.org/10.3390/nu16071070
30. Dalton, A., Mermier, C., & Zuhl, M. (2019). Exercise influence on the microbiome–gut–brain axis. Gut Microbes, 10(5), 555–568. https://doi.org/10.1080/19490976.2018.1562268
31. Cleveland Clinic. (2026, March 16). What are probiotics & what do they do? https://my.clevelandclinic.org/health/treatments/14598-probiotics
32. Shah, A. B., Baiseitova, A., Zahoor, M., Ahmad, I., Ikram, M., Bakhsh, A., Shah, M. A., Ali, I., Idress, M., Ullah, R., Nasr, F. A., & Al-Zharani, M. (2024). Probiotic significance of lactobacillus strains: A comprehensive review on health impacts, research gaps, and future prospects. Gut Microbes, 16(1). https://doi.org/10.1080/19490976.2024.2431643
33. Zhang, P. (2022). Influence of foods and nutrition on the gut microbiome and implications for Intestinal Health. International Journal of Molecular Sciences, 23(17), 9588. https://doi.org/10.3390/ijms23179588
34. Shah, S. S., Noman, O., & Jaiswal, N. (2023). Unveiling the gut microbiome: How junk food impacts the gut. Cureus. https://doi.org/10.7759/cureus.49179
35. Sejbuk, M., Siebieszuk, A., & Witkowska, A. M. (2024). The role of gut microbiome in sleep quality and Health: Dietary Strategies for Microbiota Support. Nutrients, 16(14), 2259. https://doi.org/10.3390/nu16142259
36. Smith, R. P., Easson, C., Lyle, S. M., Kapoor, R., Donnelly, C. P., Davidson, E. J., Parikh, E., Lopez, J. V., & Tartar, J. L. (2019). Gut microbiome diversity is associated with sleep physiology in humans. PLOS ONE, 14(10). https://doi.org/10.1371/journal.pone.0222394
37. Triantafillou, S., Saeb, S., Lattie, E. G., Mohr, D. C., & Kording, K. P. (2019). Relationship between sleep quality and mood: Ecological Momentary Assessment Study. JMIR Mental Health, 6(3). https://doi.org/10.2196/12613
38. Exploring the impact of sleep on Digestive Health. Cleveland Clinic. (2024, October 8). https://my.clevelandclinic.org/podcasts/butts-and-guts/exploring-the-impact-of-sleep-on-digestive-health
39. Beurel, E. (2024). Stress in the microbiome-immune crosstalk. Gut Microbes, 16(1). https://doi.org/10.1080/19490976.2024.2327409
40. Centers for Disease Control and Prevention. (2025, June 9). Managing stress. https://www.cdc.gov/mental-health/living-with/index.html