
Neurodegeneration in First Responders: How Chronic Stress and Sleep Deprivation Quietly Damage the Brain
Overview:
Approximately 14 days of the month I’m awoken to the piercing sounds of sirens and bright flashing red lights. Sometimes right as my head has hit the pillow, sometimes in the middle of a dream, though most times at some wee hour in the morning in the middle of an unrestful sleep after a restless day. Its jolting. You know the dream where you’re falling, and you jerk awake as if you were falling off a roof? That’s no longer a peaceful restful situation. You are now wide awake, likely sweating and your heart is beating fast. This is what happens every time the sirens drop. Theres a wave of feelings that wash over me every time the sirens wake me up, “shit!, okay I’m awake, dammit I wish I wasn’t, where am I? Oh yeah, what time is it? Never mind it doesn’t matter. Where are my boots?” this is pretty much what goes through my head every time I’m awoken by these loud sirens and bright flashing red lights.
Can you guess what I do? I am a first responder.
Theres a moment I think we have all experienced where you wake up and don’t know where you are what time it is or even what day it is, this happens to us more frequently when we are awoken and don’t wake up naturally. This type of wakeup call elicits a stress response but may be the least stressful part of the day depending on the call. So every time those alarms go off our bodies go through a few seconds of stress before we remember where we are and who we are. I love my job, and I love sleep, so while there is that “fuck, I just laid down moment” there is also “someone needs help, and we are the help” So it doesn’t matter the time, or how good the dream was, we respond to the call always. This is the real taxing part of the job, the constant state of activation, of fight or flight, and our training is to fight. While some calls are traumatic and dangerous at time running into fires or doing CPR on the side of the interstate isn’t the most stressful part of the job. Increased stress and lack of adequate rest is one of the biggest morbidities in first responders, yet it’s rarely acknowledged.
When most people think of first responders, we think of people who operate in environments that most people only encounter in their worst moments. Being repeatedly exposed to trauma, high-stakes decision-making, unpredictable schedules, and sometimes life-threatening situations, and that’s not incorrect! What we might not think of is the toll this takes on the body and mind. The psychological toll of this work has received increasing attention, a deeper and less visible issue is emerging: the potential for long-term neurodegeneration driven by chronic stress and sleep deprivation.
This blog’s goal is to explore how the occupational demands placed on first responders may accelerate brain aging and the neurodegenerative process. By examining the biological mechanisms underlying stress and sleep disruption, we can better understand why first responders may be at heightened risk, and what can help to keep them healthy.

…
What Is Neurodegeneration and why should you care?
Neurodegeneration refers to the progressive loss of structure and or function of neurons, including neuronal death. This process underlies conditions like Alzheimer’s disease, Parkinson’s disease, and other forms of neurodegeneration. While aging is a primary risk factor, environment and lifestyle factors, especially chronic stress and poor sleep, are increasingly recognized as major contributors of neurodegeneration (1,2).
The process of neurodegeneration unfolds slowly over years or decades, often long before symptoms appear.Proteins are a major biomolecule and provide important structural components for tissues and cells. In the brain, proteins act as the building blocks that let neurons talk to each other. The way a protein folds acts as a key and blue print for its function. See here:
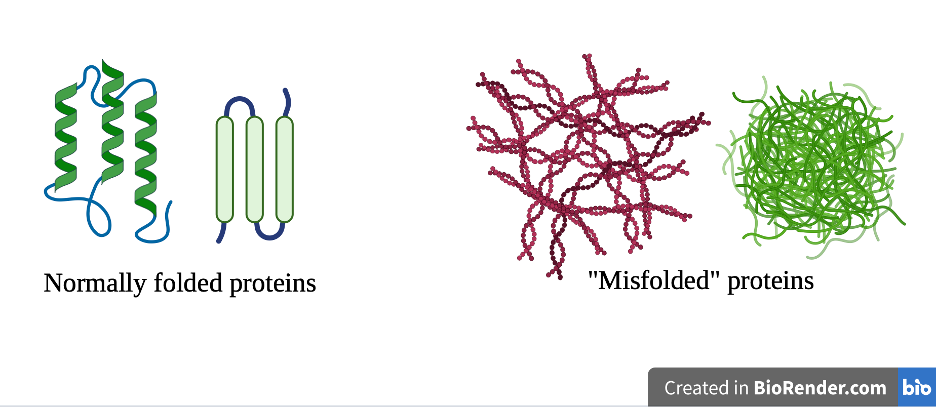
We see in this image that the normally folded proteins are “skinny” and “uniform”, while the misfolded proteins are “bulky” and “messy”. When a protein misfolds it can create these bulky deposits. Which for all intents and purposes can get stuck and impair cellular function. So, when we have buildup of these deposits, we see decreased function in our cells that are necessary for proper function! So, at its core neurodegeneration involves a combination of protein misfolding and impaired cellular repair mechanisms (2).
…
First Responders: A Perfect Storm of Risk Factors
First responders face an amalgamation of conditions that can be harmful to the brain:
- Chronic psychological stress from repeated exposure to trauma
- Irregular sleep patterns due to shift work and overnight duties
- Hypervigilance, even off-duty (like being on edge with loud sounds)
- Cumulative fatigue, often with inadequate recovery
Individually, each of these factors can affect brain health. Together, they can create a compounding effect that may accelerate neurodegenerative processes (3).

…
The Role of Chronic Stress in Brain Degeneration
Stress is not inherently harmful, in fact, acute stress is essential for survival and can boost cognition, for example encountering a bear in the woods allows you to run faster. However, when stress becomes chronic, it triggers sustained activation of the stress, leading to prolonged release of cortisol and other stress hormones.
Over time, chronic stress can:
- Damage the hippocampus, a brain region critical for learning and memory
- Increase wear and tear on your cells that weakens their structure and function impairing their ability to perform normal cellular functions. Essentially waste buildup
- Waste buildup triggers inflammation in neurons, a key driver of neurodegeneration
- Disrupt neuron’s ability to communicate with each other, impairing learning and memory
Research shows that chronic stress contributes directly to neurodegenerative processes through cellular inflammation which decreases cell’s ability to properly function. (4,5). Prolonged exposure to stress has been shown to reduce the volume of brain regions associated with learning and memory and impair neuronal survival (6).
Even more concerning, chronic stress alters neuronal immune cell function, keeping these immune cells in a constant state of inflammation that can accelerate neuronal damage (5).
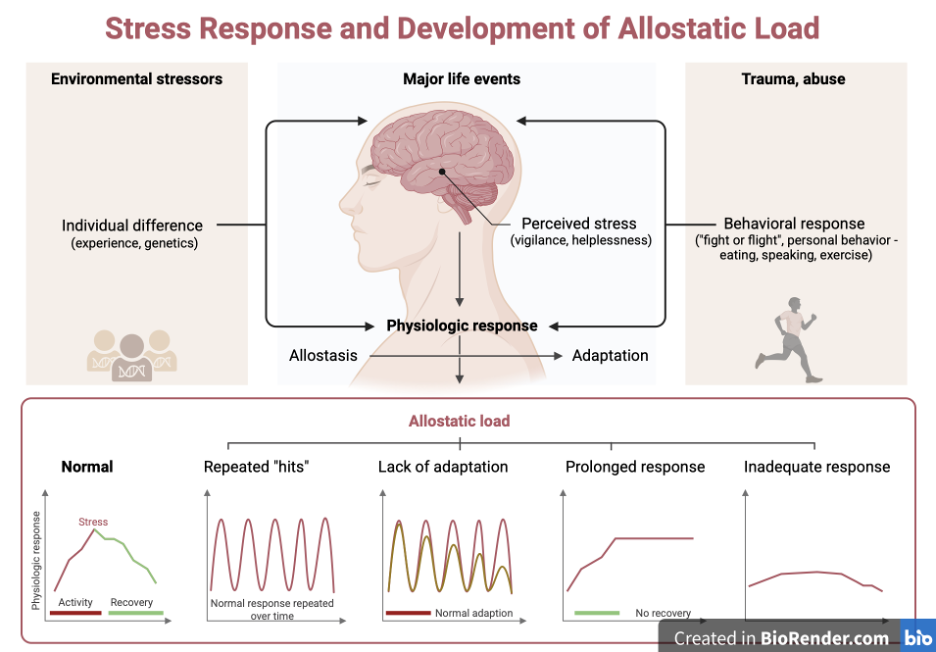
…
Sleep Deprivation: The Brain’s Cleanup System Fails
If stress is one half of the equation, sleep deprivation is the other.
Sleep is not just rest—it is an active, restorative process during which the brain clears out metabolic waste. One of the most important systems involved is the waste clearance system, which removes toxic protein build ups that contribute to neurodegeneration (7).
When sleep is disrupted or shortened:
- The brain becomes less efficient at clearing toxins
- Accumulation of toxic protein build ups that are linked to neurodegeneration
- Neurons experience increased cellular stress, impairing function
- Production of new neurons declines
Chronic short sleep, which is defined as less than 7 hours per night is associated with increased risk of cognitive decline and neurodegenerative disease (8,9). Experimental studies show that even one night of sleep deprivation can increase harmful protein build ups that increase the risk of neurodegeneration (10).
…
The Stress–Sleep Feedback Loop
Perhaps the most damaging aspect for first responders is how stress and sleep deprivation reinforce each other.
- Stress makes it harder to fall and stay asleep
- Poor sleep increases emotional reactivity and stress sensitivity
- Both together amplify inflammation and brain dysfunction
This bidirectional relationship creates a cycle of dysregulation that exacerbates neural damage over time (11). Constant activation of stress disrupts sleep, and sleep loss further activates the stress response system which increases cellular dysfunction.
…
Shift Work and Circadian Disruption
Many first responders work rotating or overnight shifts, which disrupt the body’s circadian rhythm—the internal clock that regulates sleep-wake cycles. For example, this is a picture of the cycle my department along with most others in the country run. Where each color represents a 24-hour shift. While on shift you are responsible for any calls, at any time, regardless of if your sleeping, eating showering or shitting. While there are nights you might get a full 8 hours of sleep, more than likely you’re running at least one call after midnight.
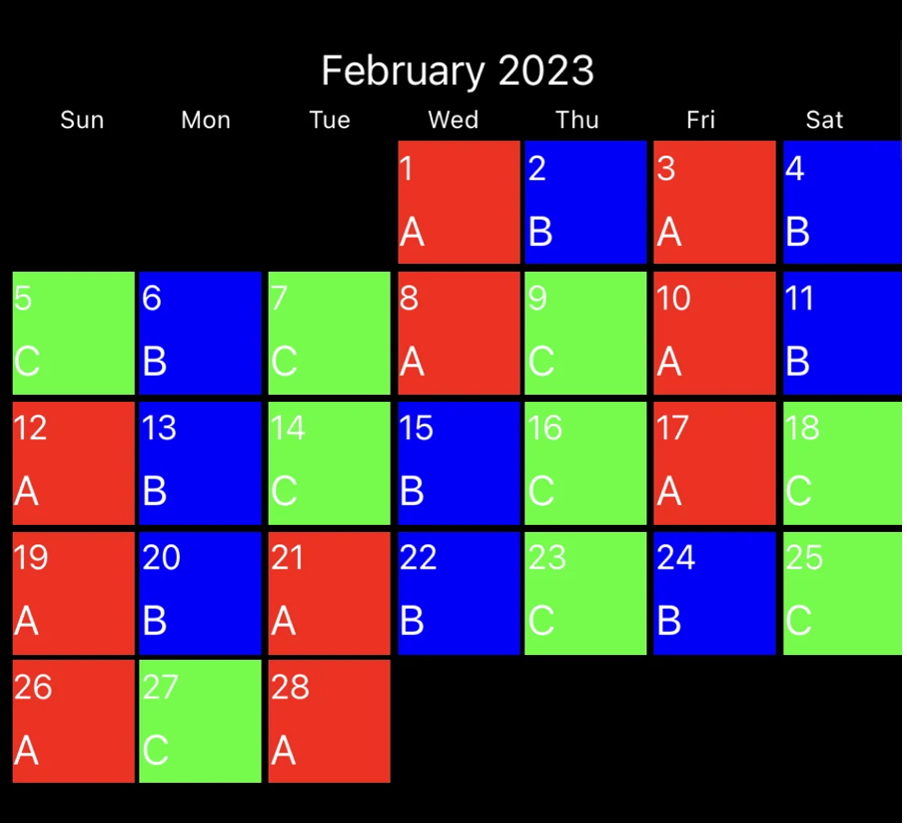
This is an example of a common schedule at many fire stations, where there are 3 different shifts, A shift (red), B shift (blue), and C shift (green). You are assigned to one shift, so say for example I was assigned to C shift I would work 24 hour shifts from 7am-7am the 5th, 7th, 9th, 14th,16th,18th,23rd, 25th, and the 27th for this month.
Circadian disruption has been linked to:
- Hormonal imbalances
- Impaired cognitive performance
- Increased inflammation
- Higher risk of neurodegenerative disease
Epidemiological studies suggest that long-term shift work may increase the risk of dementia and cognitive impairment (12).
…
Evidence from Research on Sleep and Brain Damage
Animal and human studies provide compelling evidence that chronic sleep loss can directly damage the brain:
- Repeated sleep disruption leads to loss of neurons and non-neuronal support cells in the brain
- Certain brain regions are more vulnerable to sleep deprivation
- Sleep loss influences the accumulation of Alzheimer’s-related proteins
If you don’t get enough sleep over a long period of time, you can actually damage the brain cells that keep you awake and alert and that damage can stick around even after you start sleeping more. Additionally, sleep deficiency activates cellular stress pathways commonly seen in neurodegenerative disorders (13).
…
Why First Responders May Be Especially Vulnerable
While many people experience stress or poor sleep, first responders experience both at higher intensity and frequency.
Key factors include:
- Repeated trauma exposure (e.g., accidents, violence, death)
- Sleep fragmentation rather than just short sleep
- Adrenaline-driven wakefulness, even during rest periods
- Societal barriers to seeking help or prioritizing mental health and physical recovery
Studies in law enforcement populations show elevated rates of sleep disorders, PTSD, and metabolic dysfunction, all of which are linked to cognitive decline (3).
…
Early Warning Signs
Neurodegeneration develops slowly, but early signs may include:
- Memory lapses
- Difficulty concentrating
- Emotional dysregulation
- Sleep disturbances
- Increased irritability or burnout
These symptoms are often dismissed as “just stress” or “part of the job,” which can delay intervention.
…
What Can Be Done?
Addressing neurodegeneration risk in first responders requires both systemic and individual approaches.
Individual Strategies
- Prioritize sleep hygiene (consistent sleep times, dark environments)
- Manage stress through exercise, therapy, or mindfulness
- Limit caffeine and alcohol before sleep
- Seek help early for sleep disorders or mental health concerns
A Growing Public Health Concern
As research continues to uncover the links between stress, sleep, and neurodegeneration, it is becoming clear that first responders represent a high-risk population that has been historically overlooked.
Protecting their brain health is not just a matter of individual well-being, it is essential for maintaining a functional emergency response system. Cognitive decline, impaired decision-making, and burnout can have real-world consequences not only for responders but for the communities they serve.
…
Conclusion
Neurodegeneration is not solely a disease of aging it is increasingly understood as a lifelong process influenced by environmental and occupational factors. For first responders, chronic stress and sleep deprivation create a biological environment that may accelerate this process.
The science is clear: sleep is not optional, and chronic stress is biologically damaging. Together, they form a powerful driver of brain dysfunction.
Recognizing this risk is the first step. Addressing it through policy, culture, and individual action is the challenge that lies ahead.
- DeTure, M. A., & Dickson, D. W. (2019). The neuropathological diagnosis of Alzheimer’s disease. Molecular Neurodegeneration, 14(1), 32.
- Hou, Y., et al. (2019). Ageing as a risk factor for neurodegenerative disease. Nature Reviews Neurology, 15(10), 565–581.
- Violanti, J. M., et al. (2017). Shift work and the incidence of injury among police officers. American Journal of Industrial Medicine, 55(3), 217–227.
- McEwen, B. S. (2017). Neurobiological and systemic effects of chronic stress. Chronic Stress, 1.
- Calcia, M. A., et al. (2016). Stress and neuroinflammation: A systematic review. Brain, Behavior, and Immunity, 57, 1–16.
- Lupien, S. J., et al. (2009). Effects of stress throughout the lifespan on the brain. Nature Reviews Neuroscience, 10(6), 434–445.
- Xie, L., et al. (2013). Sleep drives metabolite clearance from the adult brain. Science, 342(6156), 373–377.
- Spira, A. P., et al. (2013). Self-reported sleep and β-amyloid deposition in older adults. JAMA Neurology, 70(12), 1537–1543.
- Pase, M. P., et al. (2017). Sleep architecture and the risk of incident dementia. Neurology, 89(12), 1244–1250.
- Ooms, S., et al. (2014). Effect of 1 night of total sleep deprivation… JAMA Neurology, 71(8), 971–977.
- Meerlo, P., et al. (2008). Restricted and disrupted sleep… Sleep Medicine Reviews, 12(3), 197–210.
- Vetter, C., et al. (2018). Mismatch of sleep and work timing… Diabetes Care, 41(8), 1707–1713.
- Musiek, E. S., & Holtzman, D. M. (2016). Mechanisms linking circadian clocks, sleep, and neurodegeneration. Science, 354(6315), 1004–1008.
- Zhu, Y., et al. (2012). Selective loss of catecholaminergic wake-active neurons… Journal of Neuroscience, 32(50), 17841–17846.
