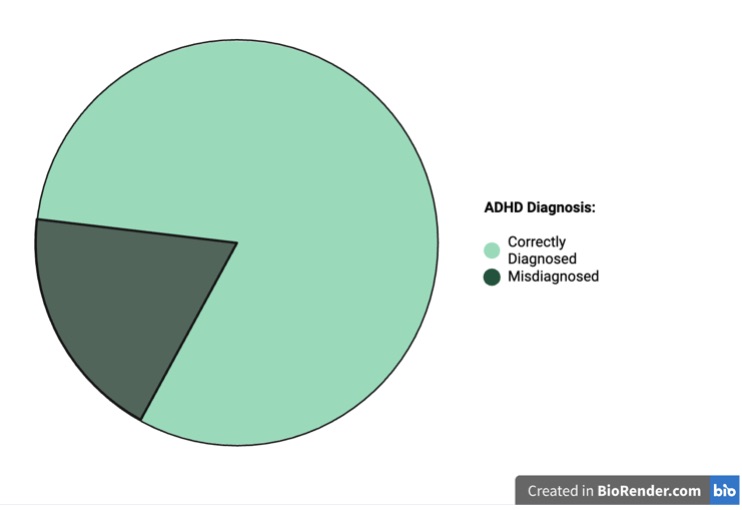
How many of you know someone diagnosed with Attention-Deficit/Hyperactivity Disorder (ADHD)? Turns out over 6 million children in America are diagnosed with ADHD in the United States alone [1]. Out of these children it is estimated that at least 1 million of them are misdiagnosed with ADHD [2]. But what is ADHD? It is a psychological problem, and people may experience trouble focusing, have a lot of movement and are not able to sit still (i.e. fidgeting), and impulsivity (not thinking through actions and thoughts and just simply doing them) [3]. This condition is considered to impact their daily lives because it is often harder for them to control their attention and focus on direct tasks [4].
To get to the point of diagnosis of ADHD for children (≤16 years old) they must have at least 6 symptoms that are related to lack of focus, hyperactivity, and impulsivity. Some examples of these are asked in questions such as [5]:
- How often does your child have trouble finishing a project or task once you complete the challenging parts?
- How often does your child fidget or squirm with their hands or feet when sitting for a long time?
- How often does your child get distracted by activity or noise around them?
- How often does your child have difficulty waiting their turn in situations when taking turns is required?
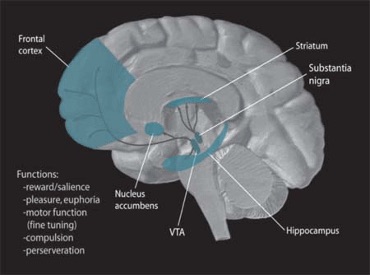
Depending on the age of the child sometimes the child will get to fill out the questions as well. But this is not always the case, meaning that the picture that doctors are getting of this child’s mental state is based off of only those around (coaches, teachers, parents, doctors) and not the child’s own interpretation of their mind. The implications of this were seen in a study from 2025 which found that out of 9708 preschool-age children with ADHD, 68.2% were prescribed ADHD medications before age 7, and 42.2% were prescribed medications within 30 days of the first documentation of an ADHD related diagnosis [6]. A problem with this approach was mentioned in this study and it was that several other psychological problems have similar symptoms to ones seen in ADHD. Some of these include anxiety, depression, learning disabilities, autism, and sleep problems [5]. Amphetamines in these cases would make the symptoms of these psychological problems worse. The brain is broken into sections called lobes, one of these lobes is called the frontal lobe. The frontal lobe is responsible for behavioral and cognitive functions. In this lobe and throughout the body there are tiny messenger cells called neurons. Neurons act like a super-fast telephone line to send information all over the body. If you look at figure 2, the blue regions show where neurons in the brain called dopaminergic neurons (they make and release dopamine) are mainly at. Since these special types of neurons are here, we also see large quantities of dopamine in these areas as well. Dopamine is a chemical messenger in the brain used to talk to other neurons. It can motivate you and gives you the good feelings you get that is associated with your reward pathway. It also helps regulate your attention. Dopamine is dysregulated in people with ADHD.
Dysregulation of dopamine in the brains of people with ADHD allows us to view those brains as an unreliable vending machine. Sometimes you put money in, and nothing comes out, or the snack gets stuck. This is like when a person with ADHD tries to invest themselves in a task, but sometimes their investment falls flat, they become distracted, and no progress is made. The snack represents the payoff—like satisfaction that comes with completing a task. Much like this terrible vending machine, the brain of a person with ADHD is unpredictable. This is similar to how dopamine works in ADHD. Dopamine helps your brain learn, “If I do this, I will get something good out of it.” But in ADHD, that signal is inconsistent, so it is harder to feel motivated to start or stick with tasks. Medication helps by making the system more reliable. It is like fixing the vending machine so that when you put money in, you can rely on it to give you a snack. Since you can rely on it you are more willing to put in effort and trust that the effort you put in will pay off. The amphetamines do not give extra rewards or make everything exciting. It just helps your brain more clearly connect effort with snacks or outcomes, which makes motivation easier. When the medication wears off, the machine cannot work as well again, and it is harder to get started on things.
One of the first things society does when it comes to an ADHD diagnosis is prescribed a pill. This pill is known as an amphetamine or more commonly as Adderall. An amphetamine is a drug that causes your nervous system to be more active [7].Adderall are used for fast acting treatment of general symptoms seen in ADHD. This drug can make you feel more focused, awake/alert, motivated, and more positive [4].

When someone takes amphetamines without needing them, they act as a powerful central nervous system stimulant that can cause overstimulation, euphoria, and significant cognitive and physical side effects. It can also lead to emotional numbness by “blocking” the surge of dopamine. Additionally, long term cognitive decline has also been seen (even though amphetamines are sometimes referred to as the “smart” drug). The misuse of amphetamines creates 3.3 times more likelihood for potential problems like coronary artery dissection (a tear in a heart artery that blocks blood flow) [8],[9]. For those who are regular users of amphetamines for the use of ADHD it may affect the brain’s ability to naturally produce dopamine due to the drugs influence, such as the lowering natural levels in the brain over a lengthened period of time since an artificial supply is being used [10]. But for those who use amphetamines and are misdiagnosed with ADHD there can be significant harmful effects. This can include lowering the natural levels of neurotransmitters like dopamine in the body’s system, and if they stop the amphetamines a drastic decline would occur [10],[11]. This decrease in neurotransmitters can put people at a higher risk for Parkison’s disease from the disruption of dopamine levels in the body by 300 percent increase [10],[12]. An increase in the risk for depression and for extreme psychosis have been seen from the use of amphetamines due to the imbalance it creates with dopamine levels [10].
But how do we know that amphetamines have an impact on dopamine and how do we visualize this? Well, with the technological advancements we have today, we can do this through what is called positron emission tomographic (PET) scan (See Figure 3). PET scans allow for you to see what happening in your body (in this case the brain) in real time. To understand how a PET scan works think of it as if your brain is playing a game of musical chairs. The chairs represent spots where signals can “sit.” At the start of the game, most of the chairs are filled by special stand-in players called tracers. These tracers are used to create images in brain scans. Now the game changes when amphetamines join. This opens the doors and lets in a huge group of players (dopamine). These players are faster and start taking the chairs. Since these players are faster, they push the placeholders (tracers) out of the seats and take them. Since we cannot see with our own eyes what the players (dopamine) are doing we use the placeholders (tracers) instead. If more placeholders lose their chairs, the PET scan shows a decrease in how many tracers remain in their “seats” at the end of the game (once the scan is finished). This decrease tells us that more dopamine is in these brain regions. From this we can further find where and how much dopamine is released in the brain [13],[14],[15].
But how do we know that amphetamines have an impact on dopamine and how do we visualize this? Well, with the technological advancements we have today, we can do this through what is called positron emission tomographic (PET) scan (See Figure 4). PET scans allow for you to see what happening in your body (in this case the brain) in real time. To understand how a PET scan works think of it as if your brain is playing a game of musical chairs. The chairs represent spots where signals can “sit.” At the start of the game, most of the chairs are filled by special stand-in players called tracers. These tracers are used to create images in brain scans. Now the game changes when amphetamines join. This opens the doors and lets in a huge group of players (dopamine). These players are faster and start taking the chairs. Since these players are faster, they push the placeholders (tracers) out of the seats and take them. Since we cannot see with our own eyes what the players (dopamine) are doing we use the placeholders (tracers) instead. If more placeholders lose their chairs, the PET scan shows a decrease in how many tracers remain in their “seats” at the end of the game (once the scan is finished). This decrease tells us that more dopamine is in these brain regions. From this we can further find where and how much dopamine is released in the brain [13],[14],[15].
While pills are used as a first step for ADHD and treating symptoms maybe we should be taking a different route before we jump to pills, especially when it comes to children. Alternative to amphetamine as a first step is cognitive behavioral therapy (CBT). CBT is a structured, informative, and goal-oriented type of therapy [16]. It aims to change patterns of thinking and behavior (cognitions) to better peoples’ moods and quality of life [16]. CBT focuses on three parts: automatic thoughts, cognitive distortions, and underlying beliefs. Automatic thoughts are immediate, unpremeditated understandings of events, these shape the individual’s emotions and actions in response to events [16]. Cognitive distortions are items that involve irrational, dramatized, or biased thoughts that negatively affect emotions and behavior. These can occur in ways such as overgeneralization, minimization, or catastrophizing [16]. Underlying beliefs are what shape the perception and interpretation of the world to each individual [16]. Having ADHD can feel like having a group of energetic monkeys in your mind. They’re curious, playful, and full of energy, but they can also get distracted easily and start jumping on the bed at the wrong times. The monkeys are not bad. In fact, their energy and curiosity can be helpful, like when you need creativity or quick thinking. The problem is that they do not always know when to settle down or focus. Cognitive Behavioral Therapy (CBT) is like learning how to work with the monkeys instead of trying to get rid of them. You learn how to notice what they are doing, catch them before they jump on the bed, and guide them to make a better choice. It is essentially having you practice by pausing for a moment and choosing what to do, instead of reacting right away without thinking about consequences and implications of situations. Instead of stopping the monkeys from being energetic, CBT helps you focus that energy in more helpful ways, like getting them to play on the floor when it is time to focus and letting them be more active when it is a more appropriate time to do so. While the monkeys do not go away with the implementation of CBT, they become easier to manage, and you feel more in control of your attention and choices. When compared to the screening process for ADHD the addition of CBT allows for a differentiation to be seen between ADHD and other disorders. The way this is done is by a therapist looking at what is the root cause of negative thoughts and actions, whether it be problems stemming from executive dysfunction (ADHD) or fear-based avoidance (anxiety). This would allow us to be able to lessen those impacted by misdiagnosis by putting another safety net while also still benefiting patients. It additionally allows for doctors to see if amphetamines are truly needed or if just CBT alone is enough. CBT Provides skills to manage habits rather than just treating symptoms like amphetamines do and has been thought to have more long-term benefits/lasting effects.
Now I am not saying to do away with pills, but that CBT should come before pills with children when it comes to ADHD. As it allows for low or no dosage of amphetamines which is better not only for the child to learn how to manage the habits but for the brain as well so it does not become dependent on this artificial DA hit. A study done by Cherkasova et al. (2016) found that with the pairing of CBT and medications showed greater improvements for those with ADHD short term compared to groups with just CBT. But, with the continuation of both groups they found that those with just CBT continued to improve while the CBT with medication group plateau [17]. Cherkasova et al. (2016) shows that while medications can resolve symptoms CBT provides an additional support or stand-alone option that allows for people with ADHD to not only treat symptoms but be able to take on and learn to manage habits.
References
[1] CDC. (2020). Page Not Found | CDC. https://www.cdc.gov/adhd/data/index-old.html?CDC_AAref_Val=https://www.cdc.gov/ncbddd/adhd/data.html
[2] Elder, T. (2010). News | MSUToday. Michigan State University. https://msutoday.msu.edu/news
[3] APA. (2025). What is ADHD? https://www.psychiatry.org:443/patients-families/adhd/what-is-adhd
[4] Cleveland Clinic. (2025b). What Is ADHD? Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/4784-attention-deficithyperactivity-disorder-adhd
[5] Cleveland Clinic. (2023). ADHD Screening: What To Expect. Cleveland Clinic. https://my.clevelandclinic.org/health/diagnostics/24758-adhd-screening
[6] Bannett, Y., Luo, I., Azuero-Dajud, R., Feldman, H. M., Brink, F. W., Froehlich, T. E., Harris, H. K., Kan, K., Wallis, K. E., Whelan, K., Spector, L., & Forrest, C. B. (2025). ADHD Diagnosis and Timing of Medication Initiation Among Children Aged 3 to 5 Years. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2838257
[7] Cleveland Clinic. (2025a). Amphetamines: What They Treat and How They Work. Cleveland Clinic. https://my.clevelandclinic.org/health/drugs/23039-amphetamines
[8] Westover, A. N., & Nakonezny, P. A. (2010). Aortic Dissection in Young Adults Who Abuse Amphetamines. American Heart Journal, 160(2), 315–321. https://doi.org/10.1016/j.ahj.2010.05.021
[9] Wu, L., Zhao, D., Lan, Y., Jin, L., & Yang, L. (2025). Comparison of serious adverse effects of methylphenidate, atomoxetine and amphetamine in the treatment of ADHD: An adverse event analysis based on the FAERS database. BMC Pharmacology and Toxicology, 26(1), 38. https://doi.org/10.1186/s40360-025-00868-5
[10] Garg, A. (2021, August 12). The Global Misdiagnosis of ADHD and the Devastating Long-Term Effects. PGHR. https://www.pghr.org/post/the-global-misdiagnosis-of-adhd-and-the-devastating-long-term-effects
[11] Schrantee, A., Bouziane, C., Bron, E. E., Klein, S., Bottelier, M. A., Kooij, J. J. S., Rombouts, S. a. R. B., & Reneman, L. (2017). Long-term effects of stimulant exposure on cerebral blood flow response to methylphenidate and behavior in attention-deficit hyperactivity disorder. Brain Imaging and Behavior, 12(2), 402–410. https://doi.org/10.1007/s11682-017-9707-x
[12] Lautiero, A., Thomas, S., Kelley, R., Stein, S., Osbourne, N., Ackerman, K.(2025). Parkinson’s Disease and Addiction. Laguna Treatment Center. Retrieved April 30, 2026, from https://lagunatreatment.com/co-occurring-disorder/parkinsons-syndrome/
[13] Drevets, W. C., Price, J. C., Kupfer, D. J., Kinahan, P. E., Lopresti, B., Holt, D., & Mathis, C. (1999). PET Measures of Amphetamine-Induced Dopamine Release in Ventral versus Dorsal Striatum. Neuropsychopharmacology, 21(6), 694–709. https://doi.org/10.1016/S0893-133X(99)00079-2
[14] Narendran, R., Jedema, H. P., Lopresti, B. J., Mason, N. S., Gurnsey, K., Ruszkiewicz, J., Chen, C.-M., Deuitch, L., Frankle, W. G., & Bradberry, C. W. (2014). Imaging dopamine transmission in the frontal cortex: A simultaneous microdiaysis and [11C]FLB 457 PET study. Molecular Psychiatry, 19(3), 302–310. https://doi.org/10.1038/mp.2013.9
[15] Weidner, L. D., Paris, A., Frankle, W. G., & Narendran, R. (2015). Safety of Oral Amphetamine Administered during Positron Emission Tomography Scans in Medically Screened Humans. PLoS ONE, 10(12), e0140647. https://doi.org/10.1371/journal.pone.0140647
[16] Chand, S. P., Kuckel, D. P., & Huecker, M. R. (2026). Cognitive Behavior Therapy. In StatPearls. StatPearls Publishing. http://www.ncbi.nlm.nih.gov/books/NBK470241/
[17] Cherkasova, M., French, L. R., Syer, C. A., Cousins, L., Galina, H., Ahmadi-Kashani, Y., & Hechtman, L. (2020). Efficacy of Cognitive Behavioral Therapy With and Without Medication for Adults With ADHD: A Randomized Clinical Trial. Journal of Attention Disorders, 24(6), 889–903. https://doi.org/10.1177/1087054716671197
