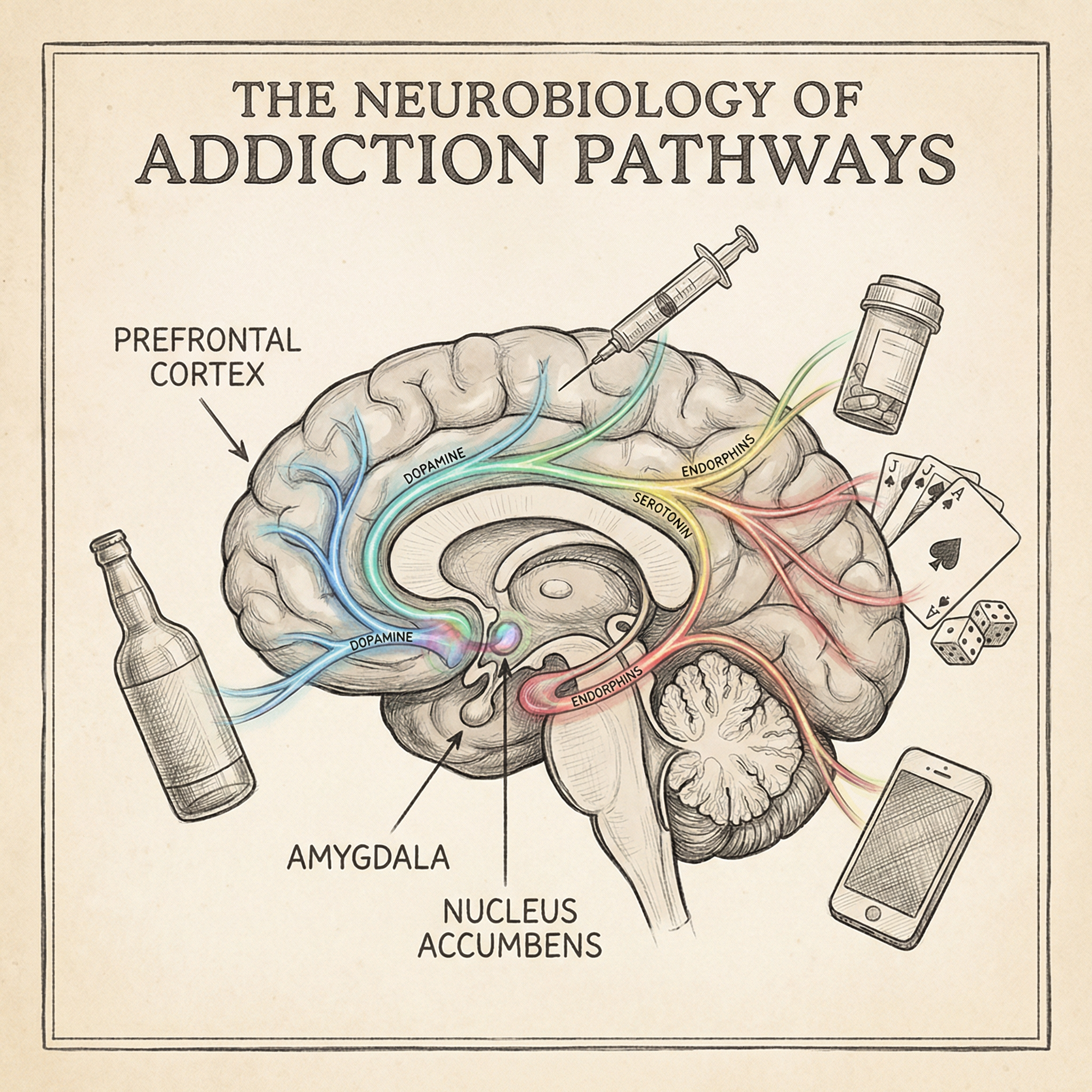
Are We Taking Behavioral Addictions Seriously Enough?
When was the last time you found yourself on the internet scrolling or gaming excessively? You promised yourself that the last time would be the last time. Yet here you are again, despite the countless promises you have made yourself. You begin to wonder how you are going to kick this nasty habit. We casually use the word “addiction” when we speak of habitual actions like eating a favorite food, and as it turns out, the line between habits and addiction can be very precarious. You might then be wondering when behaviors cross over into addictions…..
According to Merriam-Webster, a habit is defined as “an acquired mode of behavior that has become nearly or completely involuntary,” and the term drug habit is often used to denote addiction1. However, the broader definition for addiction is a compulsive, chronic, physiological, or psychological need for a habit-forming substance, behavior, or activity. Addictions typically have harmful physical, psychological, or social effects and well-defined negative symptoms during abstinence from the behavior or substance2. Sound familiar? Does this describe your relationship with your phone or someone in your life with theirs? Perhaps a certain iPad kid? The rise of the phrase “iPad Kids” has increased in popular media following the COVID-19 pandemic. The term “iPad kid” refers to younger kids who seem to be addicted to computers, tablets, and phones. As the age of the internet continues, the use of technology in our lives is inevitable. However, understanding behavioral addictions like internet addictions forces us to reconsider where to draw the line at what is considered normal and excessive use of these technologies. This, in turn, makes us better prepared to recognize and implement interventions when needed and before our medical and educational systems become overwhelmed.
I like to think of addictions as habits gone rogue, but let’s see what the science says! The DSM-5, the American guide responsible for categorizing psychiatric and psychological disorders, considers 4 categories when diagnosing a drug addiction (substance use disorder). These include:
1) impaired control over the use,
2) social impairment, which causes social and interpersonal disruptions in the lives of users,
3) risky use despite awareness of its negative consequences, and
4) physical symptoms such as tolerance and withdrawal. Tolerance is a subsequent increase in substance dose needed to achieve a previous effect with a smaller dose. Withdrawal is a collection of signs and symptoms that occurs when the levels of the substance are reduced in the body and are only relieved by using that substance3.
While these criteria have historically been used to refer to substance use disorders in previous DSM editions, the DSM-5, which is the most recent edition, recognizes that these criteria may extend to behavioral disorders as well and can be applied to broader categories of addictive behaviors4. The only officially recognized behavioral addiction in the DSM-5 is gambling disorder, but other addictive behaviors, such as Internet gaming disorder, have been listed in the DSM-5 section for conditions that require further study5. Internet gaming disorder may reflect an internet addiction or a broader problematic use of the internet overall. Although not officially listed or recognized in the DSM-5, other behaviors have been gaining traction in both the public media and the medical community.
Addictions relating to sex, exercise, food, and shopping were discussed but not included as it was concluded that there was insufficient scientific research to establish the diagnostic criteria and course descriptions needed to identify these behaviors as mental health disorders, at the time of the updated edition of the DSM5. Regardless of the lack of recognition in the DSM, many people continue to seek help for these behaviors, and higher proportions of individuals are acknowledging risky or problematic levels of these behaviors. This calls for increased research into these behaviors, and in the years since the DSM-5 was released, many researchers have been just as interested in understanding the neuroscience of behavioral addictions, and internet-associated addictions remain a top contender.
In the many years since Internet gaming disorder was identified in the DSM-5 by the American Psychiatric Association as a disorder of interest, particularly in relation to behavioral disorders, human engagement with the internet has changed significantly. We have moved from desktop-based use to phones. This means we are more connected than ever before, with several social media platforms vying for our attention and curated specifically to keep us continually engaged. The ease of access using phones has made this incredibly prevalent and easy.
In light of these changes, this article will look at similarities and differences between officially recognized addictions such as substance addictions, and gambling, and compare it to problematic internet use. Both behavioral and substance addictions often have co-occurring impairments with psychiatric disorders like depression, anxiety, and ADHD6. Many people with behavioral addictions often have an urge or craving prior to starting the behavior, as do individuals with substance use disorders prior to substance use. Additionally, Individuals exhibiting these behavioral disorders often have decreased anxiety and a positive mood or “high” after engaging in them, similar to substance intoxication. Finally, these two addiction types hijack the brain’s reward system, which is responsible for creating feelings of pleasure and motivation.
Brain Reward Circuitry
Habitual and addictive behaviors are known to hijack the brain’s reward circuitry. The brain’s reward circuitry is controlled by a neurotransmitter, dopamine. Neurotransmitters, like dopamine, are molecules released by one neuron onto another to cause different activation processes in the brain. Essentially, dopamine acts as a light switch in the brain. A room with multiple switches can have different lighting settings depending on which switches are on. Similarly, the brain lights up based on where dopamine is released to switch on the neurons.
Dopamine is manufactured and stored deep within the deep brain structures, which act as warehouses. The neurons that release dopamine serve as the delivery guys that drop their packages off to where they have been ordered: the frontal cortex, which is responsible for higher-order thinking, the hippocampus, responsible for memory making and retrieving, and the striatum, involved in regulating habit formation and voluntary movement. The striatum is critical in the transition from habits to addiction. Below is an image showing where dopamine is made and released in the brain.
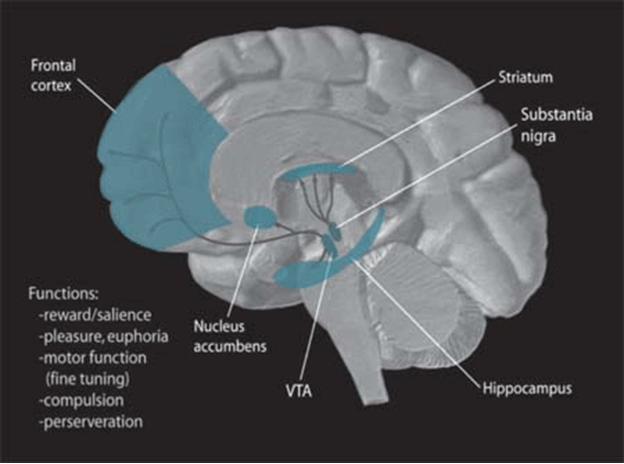
In recent years, the neurotransmitter dopamine has made its way into popular culture, particularly when talking about things that make us happy. It isn’t uncommon to come across a content creator while scrolling on TikTok telling you how to “hack” your dopamine to make you happier or more focused (or maybe that’s just what my for you page looks like). Commonly known as the “feel-good” neurotransmitter, dopamine is increasingly associated with social media use and is often categorized as either good or bad. It isn’t an inherently bad molecule, as it keeps us happy and motivated to do the things that are important to us or make us happy. However, like all things in the body, too much of it or too little of it disrupts the balance of the body, and dysregulation of dopamine in the brain can cause several problems, with addiction being one of the top contenders.
In particular, the striatum and a part of the frontal cortex called the prefrontal cortex are differentially activated in internet and gambling disorders. Researchers looked at activation across multiple brain regions using a technique called fMRI. fMRI is a pretty interesting brain imaging technique that has been used in multiple studies in neuroscience. It measures activity across the brain. Specifically, when neurons fire or are activated, they utilize a lot of energy, which means they consume a lot of glucose and oxygen, both of which are necessary for the creation of energy molecules in cells. The body increases blood flow to the brain regions that require more oxygen when these neurons are active. Blood flow is subsequently measured and mapped using a machine that creates a 3D image of the brain, creating an fMRI image. In the fMRI image, the more an area is activated, the brighter it appears in the 3D image.
fMRI studies have established that parts of the pre-frontal cortex and the striatum, both usually activated by dopamine, have increasingly less activation in gambling and cocaine addicts compared to non-addicts7. This indicates that the neurons in these regions are firing less than they usually would in response to dopamine. In fact, the higher the striatal deactivation, the higher the severity of the gambling addiction. Similarly, researchers have observed that individuals with Internet Gaming Disorder also show reduced/impaired activation in parts of the striatum and the prefrontal cortex8. This reduced activation observed, particularly in the prefrontal cortex, may cause impulsiveness, loss of motivation, impaired memory, planning, judgment, and staying focused9.
How then does differential activation of these brain regions create addiction symptoms? If your light switches stop working, or if there is a power outage, what is the first thing you do? You automatically reach for the nearest light source, perhaps a flashlight. These behaviors or drugs are simply the flashlights. When addicted, not enough of your natural dopamine is being produced, and your dopamine no longer switches on neurons in these areas at the normal level. Drugs and behaviors that increase your dopamine become things that addicts engage in to bring them back to normal activation and make you feel normal10. This represents why addictions are so hard to stop, because they aren’t making you just “high”, they make you feel normal. These dampened dopamine transmissions can be caused by either environmental or genetic factors or a combination of both.
In substance addictions, the initial habitual use of drugs floods the dopamine system and causes the body to dampen its dopamine production and response to ensure it isn’t overactivating these neurons. Similar mechanisms can be seen in behavioral addictions, where engagement in these behaviors increases the brain’s dopamine release and habitual engagement floods your dopamine system as well, eventually numbing down your brain’s dopamine transmission. Subsequently, the brain underreacts to other activities that activate its natural reward system. Other times, some people have naturally dampened dopamine transmission, such as people with ADHD and other genetically predisposed people to lower dopamine transmission. This makes them more susceptible to addiction, showing why addictions often occur with other psychiatric disorders.
As mentioned earlier, both behavioral and substance addictions take a toll on addicts’ lifestyles. Routine pharmacological and psychological treatments for substance abuse are not unwarranted. Consistent drug use and overdoses lead to death, and over 100,00 people die yearly in the United States alone due to drug addiction. Drugs have a very physical effect on other organs such as the lungs, heart, and liver. They put users at risk for a lot of other diseases, such as cardiovascular and liver diseases. They also make users more likely to be involved in accidents. Without a doubt, substance abuse has far-reaching consequences, and I do not attempt to discredit the serious harm that comes from substance abuse. However, medical help for substance addictions is a lot more prevalent than behavioral addictions.
Individuals with behavioral disorders who are actively trying to quit go through mental anguish every day. Is than not a form of silent death itself? These individuals live with shame, guilt, and long-term stress due to these disorders. Chronic stress is well known for disrupting several systems in the body, making them more susceptible to cardiovascular diseases and weakening the immune system.
They suffer a deterioration in mental health due to shame and guilt. Additionally, behavioral addictions are characterized by impulsivity and lack of inhibitory control, which makes individuals with this disorder more likely to commit suicide.
On an economic level, those with gambling addictions and internet addictions often hurt their own pockets trying to fund their addictions. Between betting and buying premium services or items for games on the internet, that’s a lot of money lost. Money that could also be used for essential things. These effects are enough to warrant more research into behavioral addictions, allowing us to study the long-term effects of them and identify commonalities between them.
Despite all these effects of behavioral addictions on the mental health of struggling individuals, many worry that expanding the classifications of behavioral addictions presents a problem of medicalizing normal human behavior. Medicalization is the process by which formerly normal biological processes or behaviors come to be described, accepted, or treated as medical problems requiring medical treatment. This suggests medical social control over people’s lives and issues. The implications of medicalization are complex; while it may reduce stigma for some individuals, it can also obscure the broader social issues that contribute to deviant behavior.
This may be a legitimate concern, but with greater internet access and a new generation of “iPad kids”, the cost to us as individuals and as a society may well be worth the risk. A buried secret or problem doesn’t disappear; it festers until it spirals out of control, and we have to curb it before it blows up in our faces. It is better to be prepared to address a growing problem by destigmatizing it. When individuals who suffer behavioral addictions such as internet addictions begin to see their problems less as moral and social failure, they are less likely to seek support, and we risk abandoning vulnerable members of our society to their fate.
If done right, behavioral addictions can be recognized without robbing them of their social context. In fact, creating awareness for internet addictions draws attention to the issue and encourages researchers to study them within different contexts and incorporate care for it into the public health sphere. So, as you begin to question habits that you can’t seem to shake. Or you notice a friend or a sibling constantly glued to their phone. Do not be shy to reach out for help when it all starts to get out of control. You may not have a behavioral disorder, but as we begin to study more about behavioral disorders, similar principles may be used to treat less severe addictions or dependencies, and we can combat this together to create a safer space for growing kids and struggling adults.
References
(1) Definition of HABIT. https://www.merriam-webster.com/dictionary/habit (accessed 2026-04-26).
(2) Definition of ADDICTION. https://www.merriam-webster.com/dictionary/addiction (accessed 2026-04-26).
(3) McNeely, J.; Hamilton, L. K.; Whitley, S. D.; Wiegand, T. J.; Stancliff, S. L.; Norton, B. L.; Gonzalez, C. J.; Hoffman, C. J. Table 3, DSM-5-TR Criteria for Diagnosing and Classifying Substance Use Disorders [a,b]. https://www.ncbi.nlm.nih.gov/books/NBK565474/table/table-3/ (accessed 2026-04-23).
(4) Grant, J. E.; Chamberlain, S. R. Expanding the Definition of Addiction: DSM-5 vs. ICD-11. CNS Spectr. 2016, 21 (4), 300–303. https://doi.org/10.1017/S1092852916000183.
(5) Potenza, M. N. Non-Substance Addictive Behaviors in the Context of DSM-5. Addict. Behav. 2014, 39 (1), 10.1016/j.addbeh.2013.09.004. https://doi.org/10.1016/j.addbeh.2013.09.004.
(6) Brand, M.; Antons, S.; Bőthe, B.; Demetrovics, Z.; Fineberg, N. A.; Jimenez-Murcia, S.; King, D. L.; Mestre-Bach, G.; Moretta, T.; Müller, A.; Wegmann, E.; Potenza, M. N. Current Advances in Behavioral Addictions: From Fundamental Research to Clinical Practice. Am. J. Psychiatry 2025, 182 (2), 155–163. https://doi.org/10.1176/appi.ajp.20240092.
(7) Potenza, M. N. The Neurobiology of Pathological Gambling and Drug Addiction: An Overview and New Findings. Philos. Trans. R. Soc. B Biol. Sci. 2008, 363 (1507), 3181–3189. https://doi.org/10.1098/rstb.2008.0100.
(8) Kuss, D. J.; Pontes, H. M.; Griffiths, M. D. Neurobiological Correlates in Internet Gaming Disorder: A Systematic Literature Review. Front. Psychiatry 2018, 9. https://doi.org/10.3389/fpsyt.2018.00166.
(9) What Does Your Prefrontal Cortex Actually Do?. Cleveland Clinic. https://my.clevelandclinic.org/health/body/prefrontal-cortex (accessed 2026-04-26).
(10) Volkow, N. D.; Michaelides, M.; Baler, R. The Neuroscience of Drug Reward and Addiction. Physiol. Rev. 2019, 99 (4), 2115–2140. https://doi.org/10.1152/physrev.00014.2018.
(11) Valenciano-Mendoza, E.; Fernández-Aranda, F.; Granero, R.; Gómez-Peña, M.; Moragas, L.; Mora-Maltas, B.; Håkansson, A.; Menchón, J. M.; Jiménez-Murcia, S. Prevalence of Suicidal Behavior and Associated Clinical Correlates in Patients with Behavioral Addictions. Int. J. Environ. Res. Public. Health 2021, 18 (21), 11085. https://doi.org/10.3390/ijerph182111085.