If you think of an iceberg, what we see above the surface of the water is just a small piece of the actual object. The water conceals most of the iceberg, allowing it to be easily mistaken as just a floating sheet of ice. Though much more complicated than an iceberg, interpretations and misconceptions of depression work in a similar way, where the symptoms we see are only a small fraction of the true story, with a wide range of symptoms and numerous neurological alterations involved. Instead, many people mistakenly view the disorder as laziness, a choice (often saying they should just choose to be happy instead), or a lack of effort (“just push through”). Similar to an iceberg, you can’t truly see mental health issues or begin to understand exactly what anyone affected is going though unless you have experienced it yourself. This lack of understanding contributes to misconceptions about these disorders. All of these misconceptions both lead to and reinforce the stigma surrounding not only depression, but mental health in general, causing additional unnecessary harm. Depression is commonly discussed in daily life and displayed in pop culture and media; however, general knowledge only reaches the tip of the iceberg. Depression alters how the brain processes information, leading to negative thinking patterns and biases, called negative cognitive biases. Depression is not just about mood, but also of brain functionality, where altered neural circuits and biases shape how people perceive, interpret, and remember their experiences. Understanding how depression affects us cognitively can help improve and personalize our approaches to treating it.
Negative Cognitive Biases- a Filter for the World
Something similar among all depressed individuals is that they have common thought patterns that guide their reasoning. Negative cognitive biases are automatic and systematic errors in thinking that are heavily influenced by negative perspectives on themselves and the world (1). People with depression tend to unintentionally process more information that confirms and reinforces these perspectives than information that challenges them. This creates a cycle where negative beliefs are confirmed by seeing the world through these beliefs (2). In a way, these biases work like a filter or a sieve, where the world is being poured into the sieve each day. The sieve is how information is processed and the negative patterns in attention, interpretation, and memory which create these biases. Often, the positive events get stuck in the sieve and don’t make it through to the brain to be processed, while the negative events run straight through like water. This allows for an increased focus on negative stimuli that confirm negative beliefs, such as “I am a failure.” With this being a core belief, it biases a person’s attention, interpretation, and memory towards stimuli and events that confirm it, such as making the person focus on all the times they failed at things they’ve tried while ignoring all the times they have succeeded. This perpetuates depressive symptoms over time and is why many people with depression feel stuck (2). Additionally, the hippocampus may, through interacting with the amygdala, activate the replay of negative stimuli, like a sort of echo, encouraging rumination (3). These patterns and altered circuits often lead to maladaptive coping mechanisms and reinforcement of depression.
Altered Brain Circuitry and its Supporting Role in Depression and Thought Patterns
The amygdala oversees emotional processing and detecting threats, especially for fear (Murphy et al., 2003, as cited by, 3). However, in those suffering from depression, structural abnormalities have been found in this area, such as reduced grey matter volume, meaning there are less cell bodies located here (Sacher et al., 2012, as cited by, 4). Additionally, the amygdala is often hyperactive (meaning more active than usual) in people with this disorder, which affects the way emotions are processed (4) by contributing to a stronger response to negative stimuli (Kanske et al., 2012, as cited by, 4). This may be the reasoning behind a higher sensitivity to negative events and emotions, shifting them into focus more than they typically are (5). People with depression often view their life through a distorted lens that zooms in on the negative, maximizing it in focus and importance, but zooms out on the positive, minimizing its importance. In the amygdala, learning occurs associating negative stimuli with negative emotions. In depression, a hyperactive amygdala creates stronger associations between these stimuli and negative emotions, causing distress when the person is presented with an unfamiliar negative stimulus (Chau & Galvez, 2012, as cited by, 3). This may cause increased sensitivity to negative information.
The hippocampus, the center for memory formation, consolidation (storing it in different places in the brain), and recollection is also involved in depression (3). Jiang (2026) also mentions many studies found through brain imaging that people with depression have an improperly functioning hippocampus. The hippocampus is also affected by the amygdala’s hyperactivity and may strengthen negative memories while decreasing access to positive memories (3). This may be the reasoning behind why people with depression often believe that nothing good ever happens to them, as their brains just have a harder time accessing the positive. Additionally, the amygdala and hippocampus interact with each other, which may strengthen the storage of negative memories (3). Stronger negative memories make them easier to recall, making the person feel as though there is no good for them in the world.
The prefrontal cortex (PFC) contributes to the regulation of executive functions (Friedman & Robbins, 2022; Girotti et al. 2018, as cited by, 6). Executive functions include working memory (which is when information is temporally held and manipulated for tasks such as problem-solving, decision-making, and comprehension), cognitive flexibility (adapting to your environment, switching gears, empathy), and inhibitory control (controlling your thoughts and thought patterns, emotions, and focus, such as resisting the urge to yell when you get angry) (7). In depression, certain areas of the PFC have a reduced volume, which may be partially responsible for the reduced cognitive control and difficulties with emotional regulation seen in depression (7, 8). Reduced cognitive control can make it harder to reframe negative thoughts, and decreased emotional regulation can make it harder to inhibit emotional responses to stimuli. This dysfunction may be partially responsible for why those with depression tend to struggle with escaping negative thought patterns, often finding themselves catastrophizing and going down a negative thought rabbit hole, one bad thought leading to another. The PFC also plays a role in regulating the activity of the amygdala, however, in those with depression, the PFC struggles to exert its inhibitory control over the amygdala, likely leading emotional reactions to dominate decision making, is associated with lower dopamine levels, and anhedonia (lack of ability to experience pleasure from normally enjoyable activities) (3, 6). Altogether, these deficits and changes make depression feel like a default and inescapable.
Together, the amygdala, hippocampus, and PFC form a network that works together to exercise regulatory control over each other and interact with one another. Evidence suggests that in depression the hyperactive amygdala may affect what information is consolidated in the hippocampus, specifically by strengthening negative emotional memories. This increased activity in the amygdala also affects the hippocampus, which strengthens negative memories while making it harder to reach positive memories (3). This unequal representation of stimuli and memories may be a contributing factor as to why people with depression tend to believe that nothing good ever happens to them, because the good is simply more difficult to access. The PFC contributes to this circuit by likely reinforcing these negative interpretations and thought patterns, as cognitive control fails to override them (3).
How Do We Know All This?
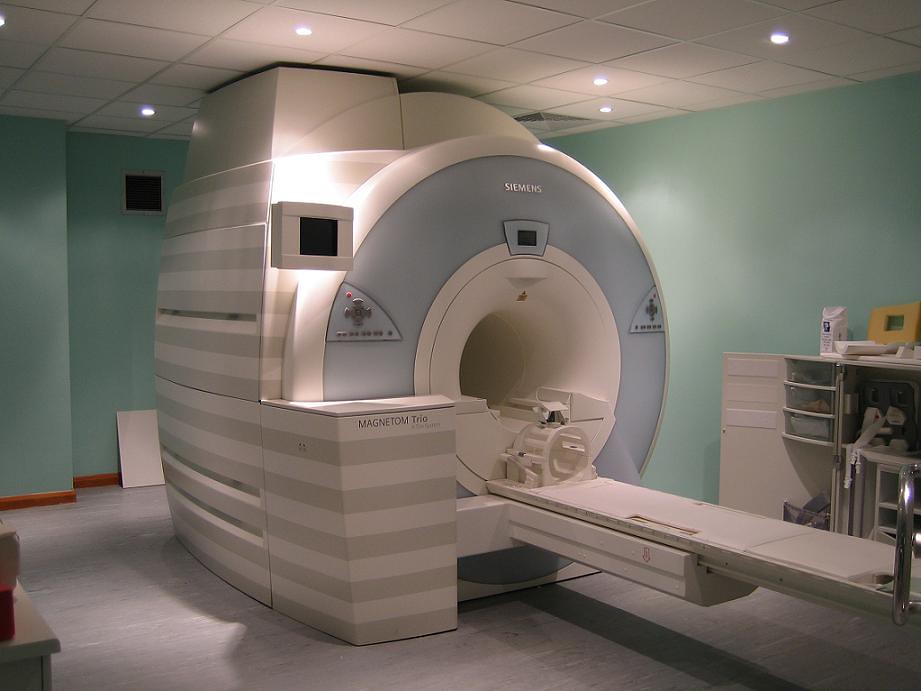
Researchers use a number of different techniques to better understand the brain, one of which is fMRI, or functional magnetic resonance imaging. An fMRI works similarly to an MRI, which uses powerful magnets and radio waves to view structures in the body (9). In an fMRI, images are captured of the brain while you’re performing a certain task, such as wiggling your fingers or imagining you’re at the beach. This is indicated by detecting the BOLD, or Blood Oxygen Level Dependent signal (4). Basically, the fMRI overlays a color-coded map of brain activity over top of the pictures it takes of the brain, showing which regions are activated while performing the instructed task (4, 9). This method is utilized in studying depression and negative cognitive biases to detect certain differences between those with depression and those without depression, such as differences in activation in response to emotional and cognitive stimuli and hyperactivation of the amygdala. These patterns point to potential reasoning behind negative emotional biases, difficulty regulating negative emotions, and rumination (getting stuck thinking or feeling negatively). Additionally, fMRI allows researchers to see the exact connections between brain regions that fail to function properly in depressed individuals (4). These changes prove that depression isn’t a personal choice or laziness; it is deeply rooted in neurobiology.
A Chemical Imbalance
In addition to altered brain circuitry, neurochemical mechanisms play a part in depression. This aspect of the disorder is much more well-known than the others, often taught in psychology or introductory neuroscience classes. However, it only provides a portion of the picture. People with depression have several neurotransmitter-related abnormalities (8). Neurotransmitters are small chemical messengers that are released from one neuron to communicate with another neuron. Most notably, this theory focuses primarily on serotonin, a neurotransmitter heavily involved in mood regulation that was orignially thought to be decreased in those with depression. However, more recent research suggests that this theory is an oversimplified version of what is actually happening (5). Other neurotransmitters are also involved in contributing to depressive symptoms, including norepinephrine, dopamine, GABA, and Glutamate (8). Norepinephrine is involved in the fight or flight stress response and vigilance and is thought to be responsible for some of the physiological symptoms of depression, such as energy, sleep, and appetite (5). Dopamine is associated with reward, motivation, pleasure, and goal-directed behavior. Depending on the area, both too much and too little dopamine play a part in depressive symptoms (5). GABA, known as the primary inhibitory neurotransmitter, has been found to be lower in some individuals with depression, likely contributing to anxiety (8, 5). Glutamate is the primary excitatory neurotransmitter and has been shown to be present at lower levels in those with depression (8). The balance between GABA and glutamate is essential for the brain to function properly, and when this balance is thrown off, as is the case in depression, it allows for circuit abnormalities, such as those previously mentioned (5).
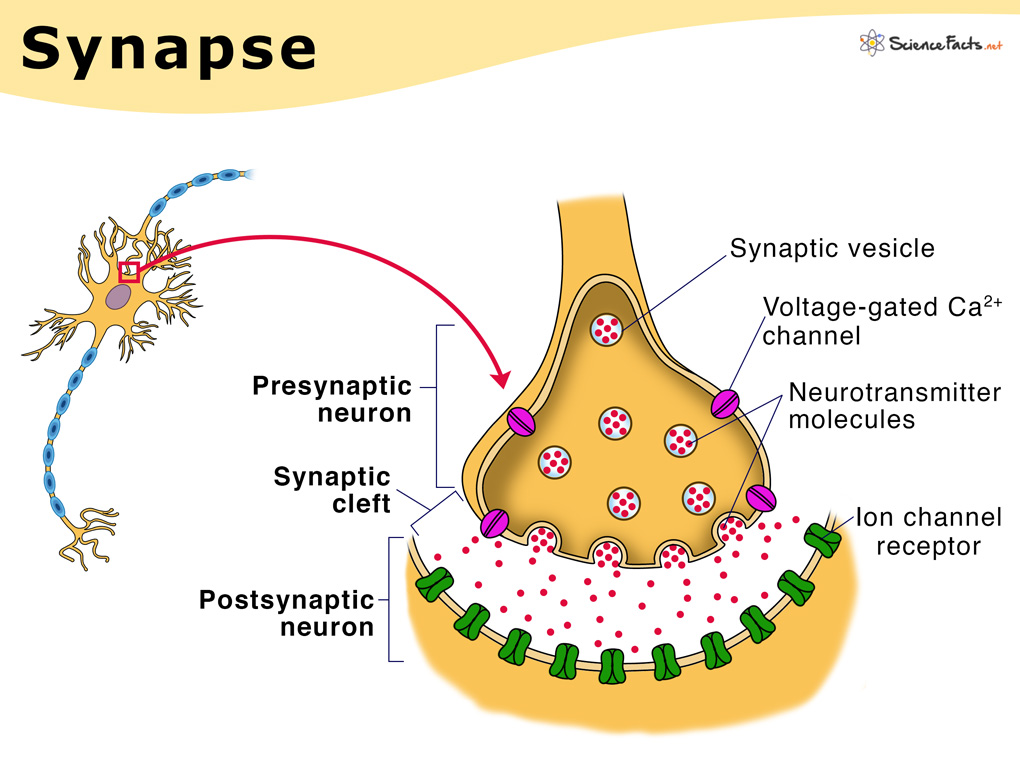
Figure 2. A synapse during synaptic transmission, which is how neurons communicate with each other using neurotransmitters such as norepinephrine, dopamine, GABA, and glutamate, which are all involved in the in depression. Image Credit: 1,600+ synapse diagram stock photos, Pictures & Royalty-free images. iStock. (n.d.). https://www.istockphoto.com/photos/synapse-diagram
Why Depression is Such a Struggle to Overcome for Many Individuals
As previously mentioned, the brain is wired to not only think negatively, but also self-perpetuate and reinforce these thinking patterns, creating a vortex of bad that feels inescapable. The brain’s reduced ability to regulate itself contributes to these feelings, as negative thoughts just seem automatic as the PFC struggles to override them. This is why “just think positive” doesn’t really work, because for those who are depressed, it is much harder to think positively than it is to think negatively. In order to do so, they must rewire their brains by continuously challenging negative thoughts, until eventually they begin to believe them, which is much easier said than done. Combined with increased recall of negative memories, it is hard not to get stuck in depression, as it feels inescapable (3). Therefore, people with depression should not be blamed, since a lot of the symptoms are out of their control and very difficult to escape.
How This Informs Treatment
Understanding the mechanisms behind why depression is so burdensome can help to improve treatment approaches. The basis of cognitive biases and rumination being rooted in improper signaling and circuitry informs us that both cognitive and neurologically based approaches can be effective in treatment. Antidepressants can be effective in treating alterations in brain chemistry and circuitry in areas such as the prefrontal cortex and reward circuitry (10). However, treating depression is hardly ever as simple as taking a pill and feeling better. Therapy is usually recommended in conjunction with medication to treat depression on all fronts. Therapy makes use of what neuroscientists call “neuroplasticity,” which is the brain’s ability to rewire itself, creating new connections that allow for learning, adaptation to the environment, and the ability to recover from injuries. Therapy has been shown to change the brain’s structure and function in key areas of the brain involved in depression. For example, the practice of reappraisal and emotional regulation strategies has been shown to strengthen prefrontal control over emotional responses. Additionally, therapeutic practices can help reduce amygdala hyperactivity, encourage neuroplasticity due to new learning experiences, and help reshape neural circuits involved in reward processing (5).
Conclusion
Depression is a disorder based inside the brain; therefore, it is unfair to make judgements about someone’s character when none of what is going on is truly ever seen. Depression may seem simple from an outsider’s perspective; however, unless you are under the water or at least know what occurs under the water, you are only reaching the tip of the iceberg. Therefore, people without adequate knowledge on the topic may not fully understand the complexity of the issue until they see the full picture and realize depression is much larger and more menacing than imagined. Promoting such learning can promote understanding and help reduce stigma. This can help those affected feel less ostracized or alone, as none of what they are going through is their fault. It is simply how their brain processes and sees the world.
References:
- LeMoult, J., & Gotlib, I. H. (2019). Depression: A cognitive perspective. Clinical psychology review, 69, 51–66. https://doi.org/10.1016/j.cpr.2018.06.008
- Rnic, K., Dozois, D. J., & Martin, R. A. (2016). Cognitive Distortions, Humor Styles, and Depression. Europe’s journal of psychology, 12(3), 348–362. https://doi.org/10.5964/ejop.v12i3.1118
- Jiang, Y. (2026, February 26). A theory of the neural mechanisms underlying negative cognitive bias in major depression. Frontiers. https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2024.1348474/full
- Singh, M. K., & Gotlib, I. H. (2014). The neuroscience of depression: Implications for assessment and intervention. Behaviour research and therapy, 62, 60-73.
- Neuroscience of depression: Moving beyond chemical imbalance. Kaplan Therapy. (2025, June 25). https://kaplantherapy.org/neuroscience-of-depression/
- Uliana, D. L., & Grace, A. A. (2026). Prefrontal cortex dysfunction as a precipitating factor for schizophrenia and Depression. Journal of Neurochemistry, 170(3). https://doi.org/10.1111/jnc.70409
- professional, C. C. medical. (2025b, December 22). Executive function: Skills for life. Cleveland Clinic. https://my.clevelandclinic.org/health/articles/executive-function
- Kaltenboeck, A., & Harmer, C. (2018). The neuroscience of depressive disorders: A brief review of the past and some considerations about the future. Brain and Neuroscience Advances, 2, 2398212818799269.
- 1.Pedersen, T. (2021, December 13). What Is fMRI? Uses, How It Works, Duration, and What to Expect. Psych Central. https://psychcentral.com/lib/what-is-functional-magnetic-resonance-imaging-fmri
- Yin, H. (n.d.). Neuroscience of depression and treatment – new frontiers psychiatry & TMS | milwaukee psychiatrist. New Frontiers Psychiatric & TMS. https://www.newfrontierspsychiatry.com/neuroscience-of-depression-and-treatment/
- Noworyta, K., Cieslik, A., & Rygula, R. (2021). Neuromolecular Underpinnings of Negative Cognitive Bias in Depression. Cells, 10(11), 3157. https://doi.org/10.3390/cells10113157
